Why it’s important
Nearly one in three people with hepatitis C are unaware of their infection status, and approximately 75%–85% of people with hepatitis C don’t have symptoms.123 Without testing, they can unknowingly transmit the virus to others.
There is no vaccine to prevent hepatitis C. Therefore, the best way to prevent infection is by avoiding behaviors that can transmit the virus.
How to make decisions on whether to test or screen
Clinicians should universally screen:
- All adults 18 and older at least once in their lifetime, except in settings where the prevalence of hepatitis C virus (HCV) infection (HCV RNA-positivity) is under 0.1%.
- All pregnant women during each pregnancy, except in settings where the prevalence of HCV infection (HCV RNA-positivity) is under 0.1%.
CDC recommends one-time hepatitis C testing for people with recognized risk factors or exposures, including:
- People who currently or have previously injected drugs and shared needles, syringes, or other drug preparation equipment.
- People with human immunodeficiency virus (HIV).
- People with selected medical conditions, including people who have ever received maintenance hemodialysis and persons with persistently abnormal alanine aminotransferase (ALT) levels.
- Prior recipients of transfusions or organ transplants, including:
- People who received clotting factor concentrates produced before 1987.
- People who received a transfusion of blood or blood components before July 1992.
- People who received an organ transplant before July 1992.
- People who were notified that they received blood from a donor who later tested positive for HCV infection.
- Health care, emergency medical, and public safety personnel after needle sticks, sharps, or mucosal exposures to HCV-positive blood.
- Infants born to people with known hepatitis C.
CDC also recommends routine periodic testing for patients with ongoing risk factors (regardless of setting prevalence), including:
- People who currently inject drugs and share needles, syringes, or other drug preparation equipment.
- People with selected medical conditions, including people who receive maintenance hemodialysis.
Clinicians should test anyone who requests a hepatitis C test, regardless of stated risk factors, because patients may be hesitant to share stigmatizing risks.
Screening and testing guidelines
Clinicians should initiate hepatitis C testing with an HCV antibody test with reflex to NAT for HCV RNA if the antibody test is positive/reactive. See the complete testing sequence.
If a patient’s antibody test is positive/reactive and they also have detectable HCV RNA, they have a current HCV infection and you should counsel the patient, evaluate for treatment, and initiate an appropriate direct-acting antiviral (DAA) regimen.
Operational guidance for complete hepatitis C testing
It is important to reduce time to diagnosis, evaluation, and treatment initiation. CDC recommends that clinicians collect all samples needed to diagnose hepatitis C in a single visit and order HCV RNA testing automatically when the HCV antibody is reactive.4 When the HCV antibody test is reactive, the laboratories should automatically perform NAT testing for HCV RNA detection. This automatic testing streamlines the process because it occurs without any additional action on the part of the patient or the clinician. See complete recommendations.
Possibility of false negatives
During acute HCV infection, antibody becomes detectable at 8–11 weeks. Therefore, a patient who thinks they may have been recently exposed might not have antibody levels high enough for a positive HCV antibody test. In addition, some people might lack the immune response necessary to develop detectable antibodies within this time range. In cases like these, clinicians should consider virologic testing.56
HCV RNA testing for recent infection
HCV RNA testing is recommended for the diagnosis of current HCV infection among people who might have been exposed to HCV within the past 6 months, regardless of HCV antibody result. HCV RNA becomes detectable approximately 1 – 2 weeks after infection with HCV. Suspected exposure may be inferred from the patient’s history or the context and setting of the patient encounter (e.g., inferred potential exposure among people who inject drugs presenting to a syringe service program).
Recommended tests
Clinicians should use an FDA-approved HCV antibody test followed by a NAT for HCV RNA test when antibody is positive/reactive. Tests include:
- HCV antibody test (anti-HCV) (e.g., enzyme immunoassay [EIA]).
- Nucleic acid test (NAT) to detect presence of HCV RNA (qualitative RNA test).
- NAT to detect levels of HCV RNA (quantitative RNA test).
A reactive HCV antibody test result indicates a history of past or current HCV infection. A detectable HCV RNA test result indicates current infection.
NAT for detection of HCV RNA should be used among people with suspected HCV exposure within the past 6 months.
Clinicians should test all perinatally exposed infants for HCV RNA using a NAT at 2–6 months. Care for infants with detectable HCV RNA should be coordinated in consultation with a provider who has expertise in pediatric hepatitis C management. Infants with undetectable HCV RNA do not require further follow-up unless clinically warranted.
How to interpret screening results
Interpretation of Results of Tests for HCV Infection and Further Actions
* If HCV RNA testing is not feasible and person tested is not immunocompromised, do follow-up testing for HCV antibody to demonstrate seroconversion. If the patient tested is immunocompromised, consider testing for HCV RNA.
† It is recommended before initiating antiviral therapy to retest for HCV RNA in a subsequent blood sample to confirm HCV RNA positivity.
§ If the patient is suspected of having HCV exposure within the past 6 months, or has clinical evidence of HCV disease, or if there is concern regarding the handling or storage of the test specimen, the clinician should follow up with the patient.
Traditional diagnostic sequence flow chart
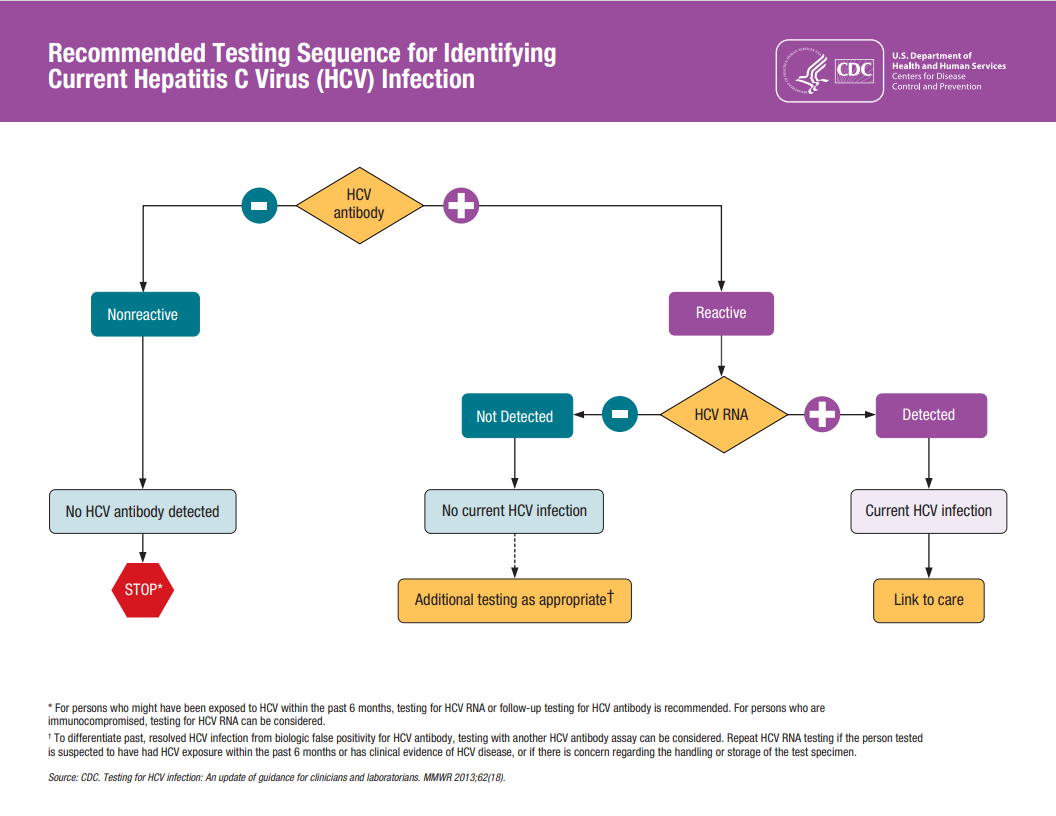
Recommended Testing Sequence for Identifying Current HCV Infection
Other resources:
CDC Hepatitis C Serology Online Training
How to diagnose Hepatitis C
If an HCV antibody test is not reactive/positive, the patient has not been exposed and you can rule out infection.
For acute HCV infection, it usually takes 8–11 weeks before antibodies are detectable.
If the antibody test is reactive/positive, you will still need to test for HCV RNA to diagnose the patient and start treatment.
It usually takes 1–2 weeks after exposure to the virus for detectable HCV RNA levels to appear.7
New guidance from CDC in July 2023 recommends complete, automatic HCV RNA testing on all HCV antibody reactive samples to minimize patient visits and increase the number of patients diagnosed and treated.
What to do next
CDC recommends that clinicians offer the following services to people who are diagnosed with HCV infection:
- Medical evaluation (by either a primary care clinician or specialist for chronic liver disease, including treatment and monitoring).
- Hepatitis A and hepatitis B vaccination.
- Screening and brief intervention for alcohol consumption.
- HIV risk assessment and testing.
More information on recommendations for testing, management, and treating hepatitis C are available from CDC and the American Association for the Study of Liver Diseases (AASLD) and the Infectious Diseases Society of America (IDSA).
Reporting cases
The National Notifiable Diseases Surveillance System (NNDSS) lists acute, chronic, and perinatal hepatitis C as nationally notifiable conditions.8
You should report cases of suspected health care-associated HCV infection to state and local public health authorities for prompt investigation and response.
When you report a case, you will use an event code that corresponds to the hepatitis C condition. You can reclassify cases if needed, as long as the changes occur before surveillance data are finalized each year.
National Event codes are:
Resources
Downloadable resources

Learn more about the Interpretation of results of tests for Hepatitis C Virus (HCV) infection and fu…
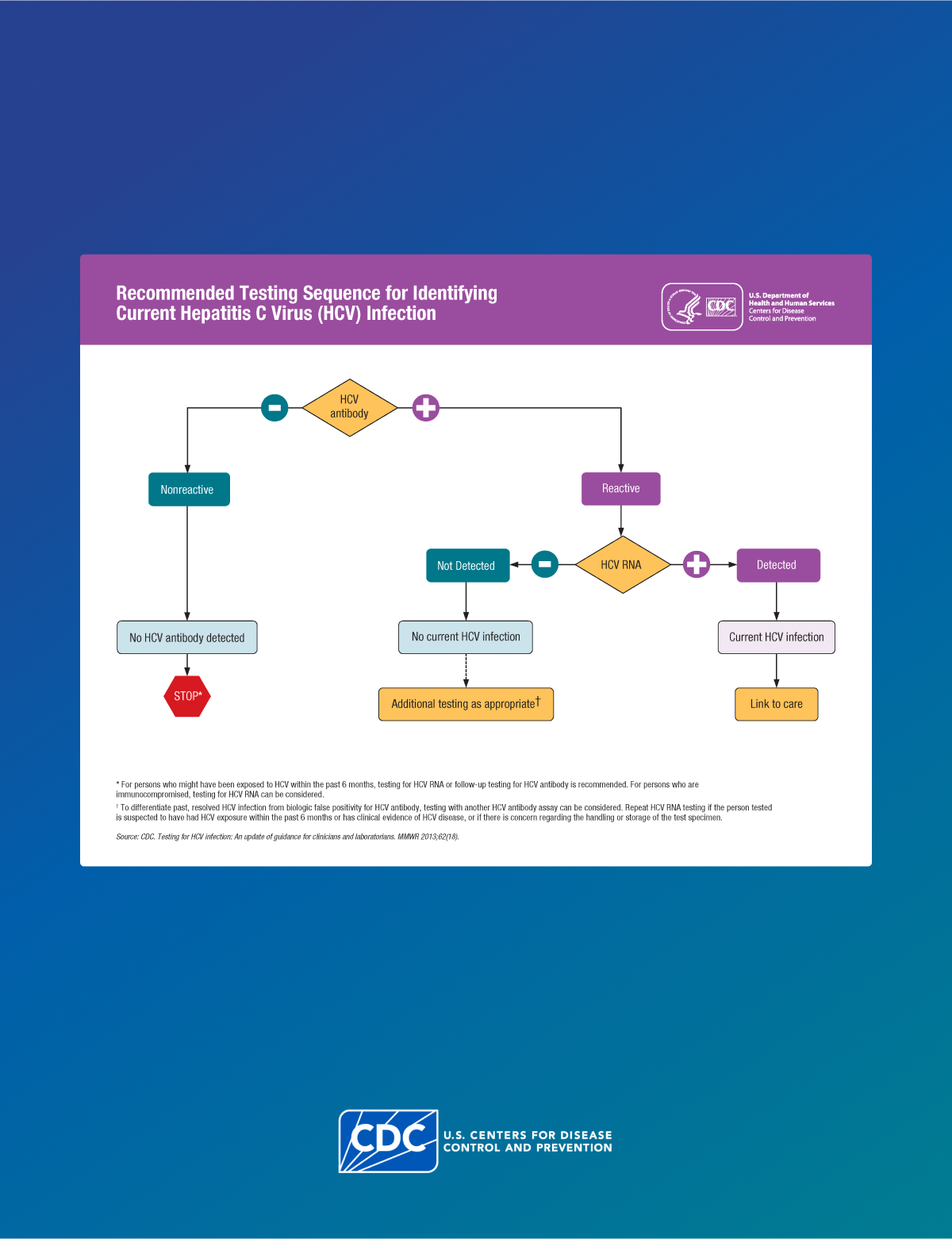
Find the CDC’s recommended testing sequence for identifying current Hepatitis C Virus (HCV) infectio…

See the CDC’s guidance for testing source patients and health care personnel after potential exposur…
Scientific guidelines and recommendations
MMWR. Morbidity and Mortality Weekly Report / Vol. 72 / No. 28 / P. 766–768
MMWR. Recommendations and Reports / Vol. 72 / No. 4 / P. 1–19
MMWR. Recommendations and Reports / Vol. 69 / No. 2 / P. 1–17
Other resources
From the American Association for the Study of Liver Diseases (AASLD) and the Infectious Diseases Society of America (IDSA).
link

